Surgery is as key as vaccination, nutrition, and mother-and-child health, says RSCI professor Mark Shrime
Dr Mark Shrime spends several weeks a year operating on tumour patients on “Mercy Ships” off the coast of Africa. He spends several further weeks a year competing in the US television contest American Ninja Warrior. You can conclude accurately from this that Shrime, the new O’Brien professor of global surgery at the Royal College of Surgeons in Ireland, or RCSI, is someone who knows what he wants from life. So, you might be surprised to hear that when he first started training as a doctor, he hated it.
“I didn’t want to go into medicine,” he says, speaking from Boston. “What I really wanted was to be a linguist. I’m Lebanese by descent. I was born in Lebanon. We are an immigrant family to the US and as the firstborn son of an immigrant family you have three options – doctor or lawyer or failure. So I chose to go to medical school. And honestly, I just hated it. I really hated medical school.”
He even went on to choose his speciality – otolaryngology, the study of diseases of the ear and throat – “for all the wrong reasons,” he says.
It was an epiphany, walking down the stairs of the ship, turning and seeing a dozen patients with head and neck tumours and thinking, Oh, this is what I’ve been training to do
“I made the decision to find something that would let me get as much money as possible but also work as little as possible so that I could do all the other things that I wanted to do, which in retrospect is a stupid way to choose your life’s career.”
Things changed for him, he says, when he first volunteered with Mercy Ships in Liberia in January 2008. Mercy Ships dock ships equipped with surgeries and medical staff off the coast of developing nations to provide much needed surgery to locals.
“It was literally an epiphany moment, walking down the stairs of the ship… turning and seeing a dozen patients with head and neck tumours and having this ‘Oh, this is what I’ve been training to do.’ After 15 years of post-secondary education, which I really hated, it just clicked.” For the first time, the path he’d taken to please his father “made sense. It hadn’t made sense to me before”.
He was further guided by a Mercy Ships surgeon named Gary Parker. “I asked Gary, ‘How do you make big life decisions?’ And he said that he looks 30 years down the road at the best possible outcome of each option. And if one of the best possible outcomes makes him think, meh, then he knows that’s not the right decision. [So] I looked 30 years down the line at being an academic head and neck surgeon at a big city hospital in the US. I was good at it and I liked my patients and they liked me, but… then I’d retire in 30 years with a nice house and a Jaguar… It just didn’t inspire me. That’s when I knew that global surgery couldn’t just be a once-a-year fly in for two weeks thing, it really had to be what my life was about.”
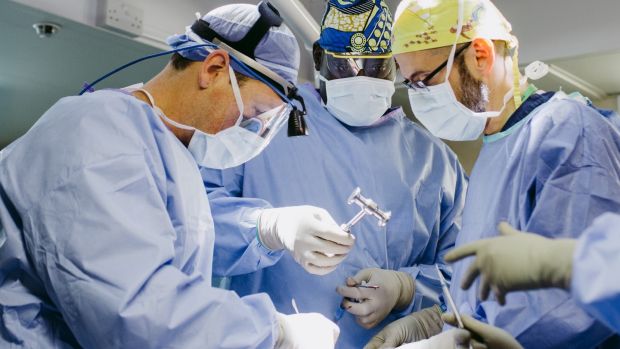
room alongside mentee Diegane Faye. Photograph: Lara Arkinstall
And it is. Shrime has co-authored the Lancet Commission on Global Surgery, founded the Center for Global Surgery Evaluation at the Massachusetts Eye and Ear Infirmary, was assistant professor of otolaryngology and global health and social medicine at Harvard Medical School and has worked and taught in Liberia, Sierra Leone, Guinea, Benin, Togo, Congo, Haiti, Saudi Arabia, Cameroon, Senegal, and Madagascar.
When it comes to international public health, he says, surgery is often overlooked. “We in the global health space, for a long time, have treated surgery as kind of icing on the cake,” he says. “Once we figure out vaccination, once we figure out nutrition and maternal and child health, then we start thinking about surgery.”
He thinks this is misguided. “When you quantify the burden of diseases as a whole around the world every year, surgically treatable conditions make up about 30 per cent of that… To give you a sort of back-of-the-napkin comparison, HIV, TB and malaria make up 10 per cent.”
He understands the resistance. Unlike disease interventions that involve distributing medicine, surgical interventions involve a high upfront cost. “Bringing surgery up to the level of other interventions means not just training surgeons and anaesthesiologists; it also means training nurses and training biomed tech-providers who can fix the machines that break. It means finding the infrastructure itself… It’s this supercomplex ecosystem.”
Here in the US and in, say, Madagascar, people are constantly making this trade off in their own minds. Should I risk going to the hospital right now, knowing it might impoverish me?
Shrime comments a lot on political issues on Twitter – the protests in the US, health inequities and the mismanagement of the Covid-19 virus. Has working in this field politicised him?
“I do think there are a lot of us who work in public health who are of the same kind of political bent, because we see how acutely decisions that we have made in the past and decisions that we make around funding and around what we focus on have very specific effects on human beings and on their health and on their lives.
“It drives a lot of us to start thinking in this kind of structural way, ‘Yes, I can fly in and spend two weeks and do some surgeries’. And I will have hopefully helped those particular patients. But I won’t necessarily have changed the underlying reason that I had to fly in in the first place.”
Patients in the US often have surprisingly similar dilemmas to those he sees in developing countries. “There was a paper that came out in 2009 that I quote all the time that said that 62 per cent of bankruptcy in the US is attributable to medical costs,” he says. “Here in the US and in, say, Madagascar, people are constantly making this trade off in their own minds. Should I risk going to the hospital right now, knowing that it might impoverish me?”
He considers the idea of being “political” for a moment. “A couple of things that I think about a lot, especially with Black Lives Matter in the middle of a pandemic, is that every choice that we make is inherently political. To choose to speak about [Black Lives Matter] is very obviously political. To choose to interrogate and see and even think about the structures that underpin racial inequities in healthcare, to even talk about those structures is political. [But] to choose not to speak about this is no less political. To say things like ‘I don’t see race’ is a political statement, as well.”
Black Americans are more likely to die if they get Covid. They are more likely to be essential workers and so not able to isolate… and they’re more likely to be shot by the police
He sees health inequality as being structurally linked to police brutality. “Black Americans are more likely to die if they get Covid,” he says. “They are more likely to be essential workers and therefore not able to isolate; their businesses are more likely to have been affected by the lockdowns and they’re more likely to be shot by the police. They are less likely to be able to access care when they need it. The fact that we see higher mortality in black Americans and Hispanic Americans in Covid, there may very well be some genetic component to that… but for sure it’s also the inevitable outcome of the structures that we have in place.”
He has also been disappointed by the US leadership’s approach to the Covid crisis. “If there’s one thing that defines Americans, it’s individualism. And we adhere to that really strongly, too strongly, in my mind, to the detriment of our collective wellbeing… Our leadership hasn’t just done nothing. They have pushed in on that. Why in the heck is it a political statement to wear a mask?… When you have a leadership that denies the existence of a pandemic, that minimises it, that says it’s nothing but the flu, those words have an effect… You see it reflected in the actions of the rest of us.”
He’s curious about why Ireland has been so much better at dealing with Covid despite only having a caretaker government until now. I spend a few minutes trying to explain our system and political culture. He once spent time in Galway as a tourist 15 years ago and has no real connections with Ireland other than a desire to head up the RSCI’s newly developed Institute of Global Surgery.
He’s been impressed by the way the college has trained surgeons in tandem with the College of Surgeons of East, Central and Southern Africa and developed new ways of delivering quality surgical care to patients in that region.
“There’s been this organic growing up of a global surgery movement within the RCSI, but for them to decide, that ‘We are going to prioritise this, this is going to be one of our pillars, to attract students and researchers specifically around global surgery,’ that’s a bold and risky commitment and shows some real leadership… And to walk into a position like that, where everybody seems to be on the same page, it was an opportunity that I couldn’t pass up.”
One thing made him hesitate. The new RCSI professor of global surgery is also a three-time contestant on American Ninja Warrior, a US version of a Japanese programme, in which contestants traverse a gruelling obstacle course.
“I’m not going to lie, it was one of the hardest things to consider giving up, to come for this job.”
How did he get involved in it? “I was watching some episodes at one o’clock in the morning – when all the best decisions are made,” he says. “And I was, like, ‘I can do this.’ They get 75,000 applications a year and I was a 41-year-old nerdy surgeon from Boston – but they called me.”
He had been a recreational climber for seven years at that point but he still found it gruelling. Ultimately, he was hooked. “I did alright in my first season. I did absolutely terribly last year, like, genuinely awful. But that’s the nature of the sport… You get up on the obstacle course and the minute you fall. That’s it. You’re done.”
It’s good to fail sometimes, he says. “One of the pieces of advice I give to doctors coming up through the system is to take up activities that are inherently risky – not risky to your life but things at which you will fail. Once you get on the medical training path, you’re on this path that’s been prescribed for you from high school to retirement. And we aren’t used to failing.
“Besides the athleticism, the thing that Ninja has given me most is a comfort with taking these risks, comfort with, honestly, flying to a country where I’ve basically never been to take a leadership position in an institution I don’t know.” He laughs. “The RCSI doesn’t know this, but one of my goals is to start Irish Ninja Warrior.”